CBS News Live
CBS News Texas: Local News, Weather & More
Watch CBS News





A tornado watch has been issued for much of North Texas, including the metroplex until 10 p.m.

"Jesus was with me. He led me there."

The Olympic flame arrived in France aboard a 19th century tall ship to kick off a 7,500-mile journey to the Paris Summer Games.

Another professional women's sport is coming to town.

Wednesday in North Texas will be a hot one — high temperatures are forecasted to be in the low 90s, according to CBS News Texas meteorologists.

Stars goalie Jake Oettinger stopped 22 shots, ending his six-game streak of allowing two goals or less.

Game 2 will be Thursday night in Oklahoma City.

Lucas Warren's birthday invitations went out last week for his fifth birthday party. There will be no party because he got killed in a flash flood Sunday morning.

Some Jewish students at the University of Texas at Dallas said walking on campus is a stroll into antisemitic verbal attacks and even getting spit on. Disagreement, they said, doesn't have to compel this behavior.

CBS News Texas anchor Doug Dunbar sat down with Fire Division Chief Daniel Williams and Police Lieutenant Kris Wirstrom to talk through that day, both professionally when it came to the response, but also personally.

The 97-year-old is one of 19 individuals who received the nation's highest civilian honor Friday.

CBS News Texas has new information from the Allen Police Department about its investigation into the outlet mall shooting that reveals for the first time the massive amount of manpower that responded to the scene.
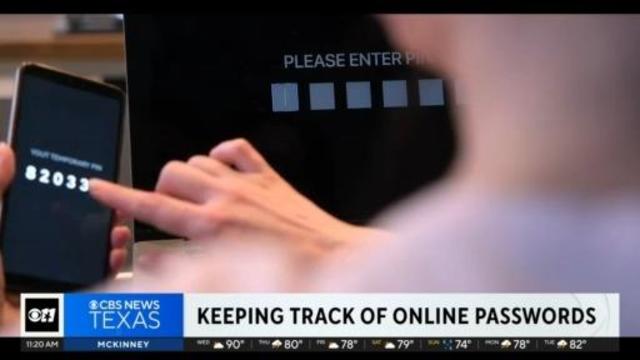
Cyber attacks are becoming more common and experts say strong passwords can protect you, but many don't follow that advice.

Apple unveiled a new lineup of iPad Pro and iPad Air tablets, as well as an Apple Pencil Pro. Devices will be in stores next week.
Large hail, damaging winds and an isolated tornado are all possible.
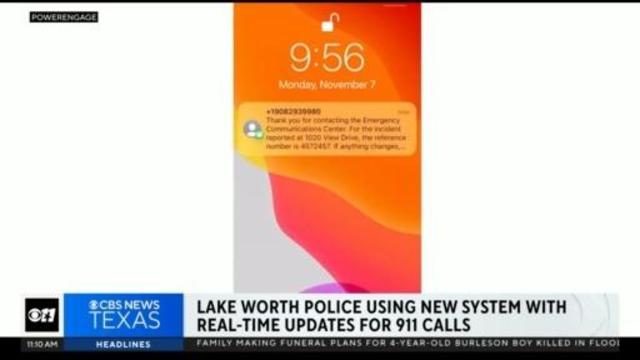
The Lake Worth Police Department is making sure emergency calls are swift and thorough, with a new system to give you real-time updates during emergencies. After you call 911 you will get a text message with the responding officer's arrival time and instructions on what to do until the officer arrives, along with a follow-up text after the officer leaves.

Dallas police are paying respects to their brothers and sisters in blue who were lost in the line of duty. The department shared a video on social media, saying it is eternally grateful for the fallen officers' service and sacrifices.

Large hail, damaging winds and an isolated tornado are all possible.

Wednesday in North Texas will be a hot one — high temperatures are forecasted to be in the low 90s, according to CBS News Texas meteorologists.
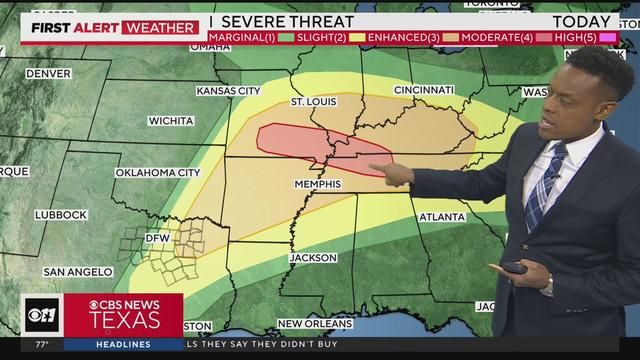
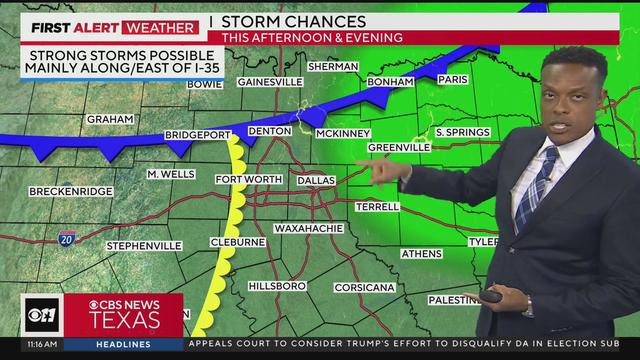
A few isolated strong to severe storms are possible, mainly along and east of I-35 late Wednesday afternoon into the evening. Large hail, damaging winds and an isolated tornado are all possible. Highs will be in the low 90s.

A Garland woman was surprised when she received a $97,000 bill for solar panels she doesn't have.
In a statement, Philips said it does not admit any wrongdoing but chose to settle "to end the uncertainty associated with litigation in the U.S."

A scammer a North Texas woman met on Instagram claimed to be a German cardiologist, and for months, the two messaged back and forth, building what she thought was a true relationship.

Texas police departments have the discretion to determine the frequency and extent of additional driving training for their officers. While some require driving training yearly or every other year, others do not.

Some departments opt to melt the firearms down, while others choose to crush them. However, there are instances where firearms, or at least parts of them, escape destruction altogether.

The Olympic flame arrived in France aboard a 19th century tall ship to kick off a 7,500-mile journey to the Paris Summer Games.

Another professional women's sport is coming to town.

Stars goalie Jake Oettinger stopped 22 shots, ending his six-game streak of allowing two goals or less.

Game 2 will be Thursday night in Oklahoma City.

Corey Seager hit a three-run homer in the eighth inning and the Texas Rangers rallied past the Oakland Athletics 4-2.

A tornado watch has been issued for much of North Texas, including the metroplex until 10 p.m.

"Jesus was with me. He led me there."

The Olympic flame arrived in France aboard a 19th century tall ship to kick off a 7,500-mile journey to the Paris Summer Games.

Another professional women's sport is coming to town.

Wednesday in North Texas will be a hot one — high temperatures are forecasted to be in the low 90s, according to CBS News Texas meteorologists.

A Garland woman was surprised when she received a $97,000 bill for solar panels she doesn't have.

In a statement, Philips said it does not admit any wrongdoing but chose to settle "to end the uncertainty associated with litigation in the U.S."

A scammer a North Texas woman met on Instagram claimed to be a German cardiologist, and for months, the two messaged back and forth, building what she thought was a true relationship.

They found him guilty – now four jurors are explaining how they were convinced to convict Dr. Raynaldo Ortiz.

Texas police departments have the discretion to determine the frequency and extent of additional driving training for their officers. While some require driving training yearly or every other year, others do not.

Stormy Daniels was called to the witness stand to testify at former President Donald Trump's trial in New York on Tuesday.

Tens of thousands of migrants are estimated to be waiting in Mexico, in places like Ciudad Juárez where shelter space is limited and the conditions are sometimes dire.

The start date for former President Trump's classified documents trial was originally scheduled for May 20.

The lawsuit claims that the measure, signed into law by President Biden, is unconstitutional.

President Biden delivered the keynote address at the U.S. Holocaust Memorial Museum's Annual Day of Remembrance Celebration.

Self-driving 18-wheelers have longtime truckers worried about their livelihood and others concerned that the technology needs more testing to make sure the public is safe.

McDonald's concept restaurant CosMc's has taken its drink-focused menu to Dallas for its second-ever location.

With the country on the cusp of greeting the return of spring, a warm-weather treat is once again available for free for a limited time only.

Kelli and Michael Regan were looking for a new dog. The breeder they found online asked them to pay with gift cards.

Target, looking for ways to add sales, is relaunching its Target Circle loyalty program including a new paid membership with unlimited free same-day delivery in as little as an hour for orders over $35.

Panera is phasing out a highly caffeinated selection of lemonade beverages that's at the center of several lawsuits.

Steward Health Care, the struggling hospital group that owns hospitals in Massachusetts, Texas, Florida and other states, announced Monday that it is filing for bankruptcy.

The Texas dairy worker infected by H5N1 "did not disclose the name of their workplace," frustrating investigators.

A North Texas mother partnered with the Texas Health Resources Foundation to provide a potentially life-saving tool to at-risk pregnant and postpartum moms.

Plaintiffs have three months to vote on whether to approve a proposed legal settlement that would resolve nearly all talc lawsuits.

Within hours of the vote, the U.S. Chamber of Commerce announced it would sue to block the ban. Dallas employment attorney Rogge Dunn predicts employees will ultimately win this battle.

The closure affects both Dom's locations in Chicago, and all 33 Foxtrot stores in Chicago, Texas, and the Washington D.C. area.

Texas law SB 14 prohibits drug and surgical "gender transition" interventions for minors.

The projects are expected to create at least 17,000 construction jobs and 4,500 manufacturing jobs.

After more than 40 years in business, 99 Cents Only Stores, a discount chain, announced on Thursday that it will close all 371 of its locations and cease operations.

The Olympic flame arrived in France aboard a 19th century tall ship to kick off a 7,500-mile journey to the Paris Summer Games.

Another professional women's sport is coming to town.

Stars goalie Jake Oettinger stopped 22 shots, ending his six-game streak of allowing two goals or less.

Game 2 will be Thursday night in Oklahoma City.

Corey Seager hit a three-run homer in the eighth inning and the Texas Rangers rallied past the Oakland Athletics 4-2.

'Bob Hearts Abishola', the acclaimed comedy, is signing off after its fifth season on CBS.

Bernard Hill died Sunday at 79. The actor was known for his roles in "Lord of the Rings" and "Titanic."

"Sunday Morning" has an exclusive behind-the-scenes look at the creation of the country singer's first post-stroke song, "Where That Came From," which blends art with artificial intelligence in a recording that captures Travis' country heart.

The start of the first civil trial stemming from the deadly crowd surge at the 2021 Astroworld festival in Texas has been delayed.

"Happy 9th Birthday, Princess Charlotte!" the Prince and Princess of Wales said in a social media post with a new photo of their daughter taken by Kate.

Cyber attacks are becoming more common and experts say strong passwords can protect you, but many don't follow that advice.

Apple unveiled a new lineup of iPad Pro and iPad Air tablets, as well as an Apple Pencil Pro. Devices will be in stores next week.

Large hail, damaging winds and an isolated tornado are all possible.

The Lake Worth Police Department is making sure emergency calls are swift and thorough, with a new system to give you real-time updates during emergencies. After you call 911 you will get a text message with the responding officer's arrival time and instructions on what to do until the officer arrives, along with a follow-up text after the officer leaves.

Dallas police are paying respects to their brothers and sisters in blue who were lost in the line of duty. The department shared a video on social media, saying it is eternally grateful for the fallen officers' service and sacrifices.
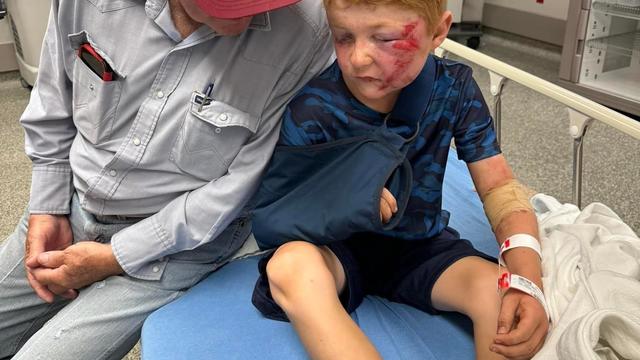
A storm chaser not only captured a massive tornado touching down in Hawley, Texas on Thursday but ended up rescuing a family of four whose home was destroyed by it.

Dallas artist Roberto Marquez traveled to the Rafah Crossing in Egypt, the U.S. capital and will attend this weekend's statewide protest in Austin.

On Friday, hundreds of thousands of fans gathered outside and all around Globe Life Field in Arlington to celebrate the Texas Rangers historical World Series win!

Babies in the neonatal intensive care unit at several Texas Health hospitals were dressed in creative costumes for Halloween.

Is that the smell of cotton candy, beignets and brisket wafting over Fair Park? It sure is, and we are here for it!