
TEA decision on Fort Worth ISD to come this fall, superintendent says
Superintendent Karen Molinar said the school district has taken bold actions for this school year.
Watch CBS News

Superintendent Karen Molinar said the school district has taken bold actions for this school year.

Texas lawmakers will attempt to make quorum Tuesday morning.

Taylor Swift announced her 12th studio album, "The Life of a Showgirl," after a countdown tease on her website. She didn't say when it would be released.

Texas Gov. Greg Abbott tells CBS News Texas there have been discussions about trying to add as many as three GOP congressional seats in addition to the five already being sought.

Burger lined a 99.4 mph pitch from Andrew Saalfrank (0-1) off the left-field wall to end the game.

Four CDC workers, who were not authorized to speak publicly, told CBS News under the condition of anonymity that they were "deeply disappointed and frustrated" by an apparent lack of leadership following Friday's shooting.

Mary Locke told jurors that she was panhandling at retail stores to support a drug addiction along with the child's father.

FIFA needs more than 6,000 volunteers for the events in the Dallas area.

Dallas public schools will welcome an expected 140,000 students on Tuesday, Aug. 12, and Elizade said she's excited.





Several organizations are accepting donations for those impacted by the floods, as well as first responders and volunteers.

Former campers, who are now adults, share their memories from Camp Mystic and remember those who died in the devastating Hill Country flood on July 4.

An act of nature has destroyed what was a kind gesture from a group of people in Parker County.

Texas officials have faced questions over their preparedness and the speed of their initial actions when flash flooding hit.

The public hearing will take place at Hill Country Youth Event Center at 9:30 a.m.

FIFA needs more than 6,000 volunteers for the events in the Dallas area.
Cheer stunts, fatherly wisdom, and an unshakable bond — that's what you'll find on Roland Pollard's Instagram feed.

The circumstances surrounding Bevers' death have remained a mystery.
Dallas ISD is returning to class on Aug. 12. Here's how the school district is making sure students are safer in schools.

Fort Worth ISD students returned to the classroom on Aug. 12. Lacey Beasley spoke with educators and FWIDSD officials to see how they prepared.
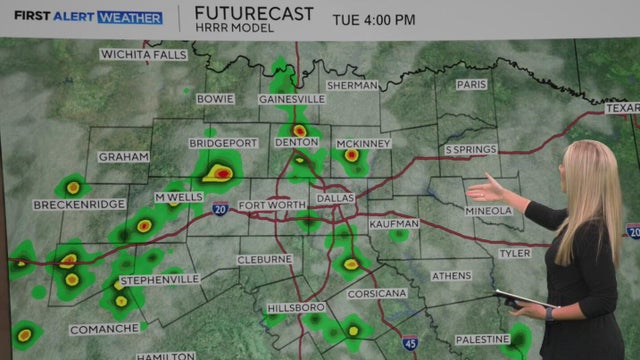
Some North Texans could get rain on Tuesday.

The U.S. and China have been working on a long-term trade deal. For now, U.S. tariffs on Chinese goods remain at 30%.

School is back in session across North Texas, which means big yellow buses are back on the roads. Here are safety tips to remember when near one.

Some North Texans could get rain on Tuesday.

As students return to the classroom on Tuesday and Wednesday in North Texas, there may be a chance you see some showers across the metroplex either dropping them off or picking them up from school.
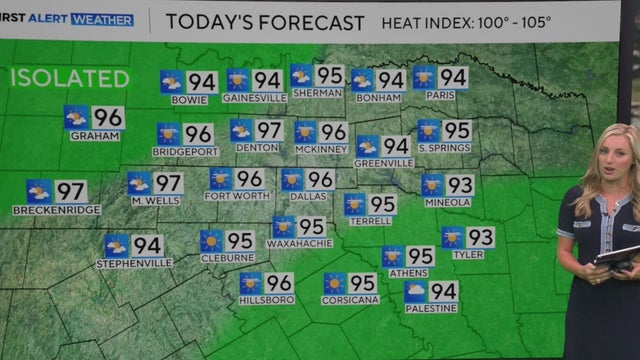
So far, 28% of this summer has been cooler than normal and this trend is likely to continue through the week.

So far, 28% of this summer has been cooler than normal and this trend is likely to continue through the week.

For migrant children, who range in age from 3 to 17 years old and arrive in the U.S. without a guardian, applying for asylum can be a confusing obstacle.

SB 36 will create a division of Homeland Security within Texas's Department of Public Safety.

Two weeks ago, the Trump administration began carrying out its latest tactic aimed at fast-tracking deportations.

The detentions come on the heels of similar arrests earlier this week in immigration courts across the country.

Multiple sources have confirmed that at least a handful of people were arrested on the spot after their cases were dismissed in Dallas.

While illegal migrant crossings have dropped, immigration courts now have a historically high volume of cases

With the expansion of the 287(g) program, local and state officers will be able to enforce some immigration duties.

While the Trump administration says they're only targeting criminals for deportation, those words have done little to comfort some immigrants

A few weeks into his second term, President Donald Trump has issued dozens of executive orders.

Burger lined a 99.4 mph pitch from Andrew Saalfrank (0-1) off the left-field wall to end the game.

FIFA needs more than 6,000 volunteers for the events in the Dallas area.

Paramount will become the new home to all UFC events in the U.S., while UFC's CEO says the White House may host a July 4 event broadcast on CBS.

Social media had a field day with the incident overnight and well into Sunday.

Shigetoshi Kotari and Hiromasa Urakawa, both 28, died after sustaining brain injuries during separate bouts on the same card at Tokyo's Korakuen Hall.
Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Eat See Play: Sponsored by Metroplex Cadillac Dealers

Superintendent Karen Molinar said the school district has taken bold actions for this school year.

Texas lawmakers will attempt to make quorum Tuesday morning.

Taylor Swift announced her 12th studio album, "The Life of a Showgirl," after a countdown tease on her website. She didn't say when it would be released.

Texas Gov. Greg Abbott tells CBS News Texas there have been discussions about trying to add as many as three GOP congressional seats in addition to the five already being sought.

Burger lined a 99.4 mph pitch from Andrew Saalfrank (0-1) off the left-field wall to end the game.

The VA in North Texas is using a new algorithm to calculate the hours of in-home care that veterans receive.

The nonprofit employs men and women who have had past run-ins with the law to work as mentors for at-risk teens and young men.

Sidhartha "Sammy" Mukherjee and his wife Sunita became known for their Bollywood-style performances, became local celebrities, hosting parties and headlining music and cultural events.

On Thursday, the Texas House and Senate announced the creation of committees on disaster preparedness and flooding.

In what experts call "Flash Flood Alley," the terrain reacts quickly to rainfall steep slopes, rocky ground, and narrow riverbeds leave little time for warning.

Texas lawmakers will attempt to make quorum Tuesday morning.

Texas Gov. Greg Abbott tells CBS News Texas there have been discussions about trying to add as many as three GOP congressional seats in addition to the five already being sought.

Huntington Park, California, is 95.6% Latino, and as many as 45% of the residents are undocumented, according to the city.

President Trump has extended a temporary truce in the U.S.-China trade war, preventing tariffs on China from leaping to at least 80%.

On Monday, Abbott spoke with CBS News Texas political reporter Jack Fink live during the 5 p.m. newscast about the political standoff in Austin.
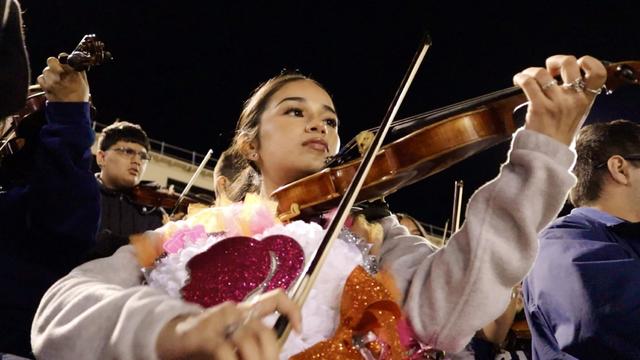
At Fort Worth ISD's North Side High School, the sounds of an American sport on the field meet mariachi music in the stands.

With new foods, such as the "Drowning Taquitos" and the "Beso de Angel," Tony's Taco Shop owners say they don't take their success for granted.

Latinas in Tech DFW started back up last year after the pandemic. They have lots of opportunities for Latinas to network, connect, and learn new skills.

Anchor Ken Molestina shows us how he makes his Cuban coffee for the CBS News Texas newsroom.

Del Olmo, who has played golf his entire life, recalls how rare the sport was for people like him growing up in Mexico City.

Less than two days after Delta Air Lines offered $30,000 to each passenger on board the flight that crashed and flipped in Toronto on Monday afternoon, the company is facing its first two lawsuits in the incident — and they likely won't be the last.

Texas Agricultural Commissioner Sid Miller is calling for a statewide ban on non-water additives, such as fluoride, in the public water system.

Last year, over 16 million vehicles drove on North Texas toll roads without paying, accumulating more than $69 million in unpaid tolls.

Activists are calling for a nationwide boycott of Target stores following the company's decision to roll back its diversity, equity and inclusion initiatives.

Discount store chain Target says it's joining rival Walmart and a number of other prominent American brands in scaling back corporate diversity, equity and inclusion initiatives.

Instagram rolled out a new Map feature that lets users see their friends' locations in real time. Here's why privacy experts are concerned.

For the first time in more than 30 years, a Fort Worth community long considered a "health care desert" now has nearby access to basic medical care.

Head Colorado Buffaloes football Coach Deion "Coach Prime" Sanders revealed his bladder cancer diagnosis for the first time on Monday morning.

Pepsi hops on another nutritional bandwagon as more consumers opt for prebiotic beverages.

Many Southeast, Southern and West Coast states are likely seeing an increase in COVID cases.

A truck had smashed through the front of Bruno's Place, destroying much of the inside.

Kroger said it intentionally decreased prices, but some customers said the financial drop at the register went in a different direction.

Could the solution to school shootings be drone first responders? An Austin-based tech company thinks so and is testing them at a private high school in Aurora.

Located off the Guadalupe River in Historic Old Ingram Loop, the shop was once filled floor to with lighting, decor and trinkets.

They were already concerned about tariffs, but construction businesses in North Texas said they have new fears with the president's immigration crackdown.

Burger lined a 99.4 mph pitch from Andrew Saalfrank (0-1) off the left-field wall to end the game.

FIFA needs more than 6,000 volunteers for the events in the Dallas area.

Paramount will become the new home to all UFC events in the U.S., while UFC's CEO says the White House may host a July 4 event broadcast on CBS.

Social media had a field day with the incident overnight and well into Sunday.

Shigetoshi Kotari and Hiromasa Urakawa, both 28, died after sustaining brain injuries during separate bouts on the same card at Tokyo's Korakuen Hall.

Taylor Swift announced her 12th studio album, "The Life of a Showgirl," after a countdown tease on her website. She didn't say when it would be released.

Prince Harry and his wife, Meghan, announced Monday that their media company's partnership with Netflix has been extended with a multiyear, first-look deal.

Paramount will become the new home to all UFC events in the U.S., while UFC's CEO says the White House may host a July 4 event broadcast on CBS.

Bobby Whitlock, the musician who co-founded Derek and the Dominos with Eric Clapton, has died, according to his manager. He was 77.

An ICE spokesperson ICE Assistant Secretary confirmed that Dean Cain will be sworn in as an honorary ICE officer in the coming month.

A suspect was taken into custody after an attack on Pearl Street Mall in Boulder on June 1 in which there were 15 people and a dog who were victims. The suspect threw Molotov cocktails that burned some of the victims, who were part of a march for Israeli hostages.

The Neonatal Intensive Care Unit babies at Texas Health locations across North Texas celebrated Valentine's Day.

As Anthony Davis prepared for his debut game at the AAC, Dallas Mavericks fans took to the arena to protest the controversial trade.

A look back at the esteemed personalities who've left us this year, who'd touched us with their innovation, creativity and humanity.

CBS News Texas viewers got out and enjoyed the snow day on Thursday and send us all of their best photos. Take a look.